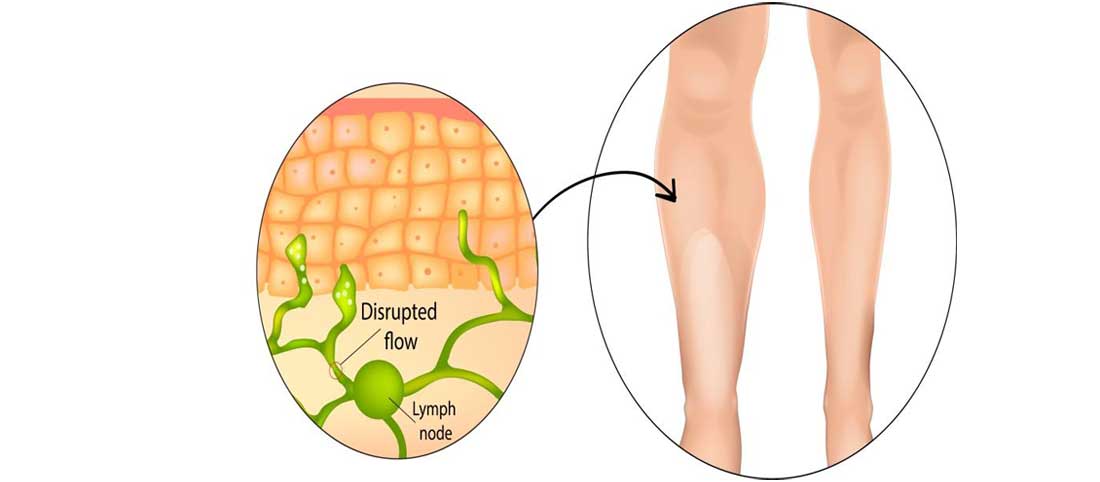
Lymphedema refers to tissue swelling caused by an accumulation of protein-rich fluid that’s usually drained through the body’s lymphatic system. It most commonly affects the arms or legs, but can also occur in the chest wall, abdomen, neck and genitals.
Symptoms:
- Difficulty with movement.
- Repeated skin infections.
- An aching, heavy feeling.
- Wart-like growths developing on the skin.
- Fluid leaking through the skin.
- Hard, tight skin
- Olds developing in the skin.
Causes:
- Infection: Severe cellulitis infection may damage tissue around the lymph nodes or vessels. This may lead to scarring, increasing the risk of lymphedema. Some parasite infections can also increase the risk of lymphedema.
- Radiation: Radiation can cause scarring and inflammation of lymph nodes or lymph vessels.
- Injury and trauma: More rarely, severe skin burns or anything that results in excessive scarring may raise the risk of developing lymphedema
- Surgery. In cancer surgery, lymph nodes are often removed to see if the disease has spread. However, this doesn’t always result in lymphedema
- Cancer surgery: Cancer may spread through the body via the lymphatic system. Sometimes surgeons remove lymph nodes to stop the spread. There is a risk the lymphatic system may be affected, leading to lymphedema.
Risk Factor:
Factors that may increase the risk of developing lymphedema include:
- Older age
- Rheumatoid or psoriatic arthritis
- Excess weight or obesity
Diagnosis:
If you’re at risk of lymphedema — for instance, if you’ve recently had cancer surgery involving your lymph nodes — your doctor may diagnose lymphedema based on your signs and symptoms.
- MRI
- CT Scan
- Ultrasound
- Lymphoscintigraphy
Treatment:

Physical Therapy
Specialized lymphedema therapists can teach you about techniques and equipment that can help reduce lymphedema swelling. Examples include:
- Exercise: Gentle contraction of the muscles in the arm or leg can help move the excess fluid out of the swollen limb.
- Manual lymph drainage: Therapists trained in this massage-like technique use very light pressure to move the trapped fluid in the swollen limb toward an area with working lymph vessels. People should avoid manual lymph drainage if they have a skin infection, blood clots or active cancer in the affected limb.
- Compression bandages: Using low-stretch bandages to wrap the entire limb encourages lymph fluid to flow back toward the trunk of the body.
- Compression garments: Close-fitting elastic sleeves or stockings can compress the arm or leg to encourage lymph fluid drainage. These garments often require a prescription to ensure that the proper amount of compression is used. You may need to be measured by a professional to ensure proper fit.
- Sequential pneumatic compression: A sleeve worn over the affected arm or leg connects to a pump that intermittently inflates the sleeve, putting pressure on the limb and moving lymph fluid away from the fingers or toes.
-
- Surgery
- Liposuction
- Debulking